The Impact of Bras on Breathing
- Nomadic Physical Therapy PLLC
- Jan 3, 2024
- 7 min read
Sport bras are designed to help reduce impact on the breasts, but what impact do sport bras have on you?
As a pelvic floor therapist (who actually practices what she preaches in the gym), I noticed it was more difficult to catch my breath during exercise when I was wearing a snug sports bra, compared to one that had a bit more compliance. With curiosity, I intentionally tried performing some diaphragmatic breathing techniques with a bra on, and then without. My initial observation: it felt much harder to take a full breath in with a band around my chest. This got me wondering, could bras be disrupting our natural breathing abilities?
It’s been speculated that up to 80% of women wear the incorrect bra size and of those women, 70% wear bras that are too small (1). A poorly fitted sports bra may fail to reduce excessive breast motion, causing breast pain and increased strain on the breast tissues. However, if the sports bra is too tight, breathing may be impaired (2).
Now you may be thinking, what’s the big deal? So what if my breathing is a little limited by my bra…I encourage you to read on and you’ll quickly see why I am fully concerned with ensuring my diaphragm functions as efficiently as it possibly can…
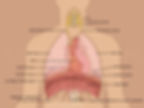
The Mechanics of Breathing
The actions of inhalation and exhalation are led by the diaphragm muscle (see image above), of which lives in the inner, lower region of the ribcage. The muscle is a dome-shaped, “fibromuscular sheet” that composes the floor of the thorax and roof of the abdomen (3).
The diaphragm is controlled by the phrenic nerve (one on each side of the body) of which originates at levels C3-C5 of the cervical spine, as well as the vagus nerve - responsible for that “rest and digest” function of the nervous system. These nerves have a complex course to navigate, starting from the spinal column, around veins, arteries, the heart, lungs and under various neck muscles before it reaches your thorax and diaphragm muscle.
Disruptions to the phrenic nerve can result in unexplained shortness of breath, recurrent pneumonia, anxiety, insomnia, morning headache, excessive daytime sleepiness, orthopnea (difficulty breathing when lying down flat), fatigue, and difficulty weaning from mechanical ventilation (4).
When the diaphragm is allowed to function normally, it acts like a piston. To allow air inhalation, the muscular dome descends, pushing the abdominal contents away from the thorax creating a negative intrathoracic pressure and expansion of the lower rib cage + abdomen. This action pulls air from the mouth into the lungs. Upon exhalation, the muscular dome recedes back upward, guiding the air out of the lungs and the ribcage and abdomen return to their resting states. This makes the diaphragm essential in the “low-intensity, perpetual cycle of breathing and in more rapid and strenuous settings, such as talking, singing, sneezing, defecation and in situations of acutely-increased ventilation” (3) such as hyperventilating during panic attacks.
So in order to function appropriately, the diaphragm requires: proper innervation from the nerves, and the ability to expand and contract within the lower rib cage. But what if a tight band around the lower rib cage disrupts the diaphragm’s ability to function well?
The Potential Impacts of Diaphragm Dysfunction
Please keep in mind this is not an all inclusive list.
Bowel Function: It has been recently proposed that an altered contractile ability of the diaphragm muscle might adversely influence intestinal motility and contribute to Irritable Bowel Syndrome (5).
Pelvic Floor Function: The pelvic floor and diaphragm are designed to move together…if the diaphragm isn’t moving well, the pelvic floor can’t either, which can result in: incontinence, pain with penetration, constipation, pelvic pain/numbness/tingling, tailbone pain, etc.
Low Back Pain: The diaphragm dynamically stabilizes the lumbar spine. Dysfunction of the diaphragm is one of the recognized causes of low back and sacroiliac joint pain. People with low back pain often experience early fatigue of the diaphragm muscle, altered and reduced excursion during respiration, and inadequate proprioceptive activation. In people with chronic lower back pain, the diaphragm remains higher and more flattened (5).

TMJ Dysfunction: The diaphragm and tongue share an intimate relationship including fascial and neurological connections. Airway abnormalities, along with coordination difficulties of the tongue, can alter kinematics of the temporomandibular joint (ie. the jaw) (5).
Chronic Headaches: Fascial and muscular connections of the thoracolumbar and abdominal regions, along with diaphragm, influence each other’s activity. Increased tension of the suboccipital muscles and/or dura mater can contribute to chronic headaches (5). It’s all one connected chain!
GERD: “The diaphragmatic crura plays a role as extrinsic sphincter in the region of the gastroesophageal junction to protect the esophagus from gastric reflux; a crural dysfunction can cause GERD” (5).
Emotions & Pain Tolerance: The interaction between breathing and emotions results from a complex interaction between the brainstem, various areas of the brain and the diaphragm. When we breathe, receptors sensitive to the physical movements of the diaphragm and visceral organs of the body send neural activity up the spinal cord, back to the brainstem and appropriate brain regions via interoception. “Interoception is the awareness of the body’s condition based on information directly obtained from the body itself. The interoception system can modulate the exteroceptive representation of the body, as well as the subject's tolerance of pain; the dysregulation of pathways managing or stimulating the interoception could cause a distortion of body image, affecting the subject's emotional state.” (5)
The Research on Sports Bras
Overall studies on this topic are scarce…in fact, I’ve found only two published to date.
In this 2005 study, researchers attempted to test whether or not sports bras affect a women’s ability to breathe at rest and during strenuous activity, tested with running on a treadmill and cycling. They documented maximal, submaximal and resting respiration status, using spirometry, heart rate, and maximal exercise performance measures. Pressure strips were placed underneath the bra band to determine “tightness”. No significant restriction to exercise performance or respiratory mechanics was found when the subjects wore sports bras (compared to no bra and fashion bra variables) (2).
Research does support the use of sports bras to reduce breast pain during physical activity (2).
A 2006 study noted that a woman's current respiratory state significantly changes bra size.
There is an average increase of one band size for chest circumferences during inhalation. Standardizing bra fitting to include respiratory state would be an appropriate step in the right direction (6).
Although the research in this specific topic lacks, I encourage you to think more broadly for a minute as I believe other components of our complex bodies may play a role.
As mentioned earlier, respiration requires proper nerve innervation. Let’s say wearing a tight bra results in an individual breathing more shallowly, utilizing their chest and neck musculature more so than diaphragmatic excursion. Overtime, hypertrophy or increased tone of the cervical muscles and pectorals could reduce the amount of freedom the phrenic nerve has to glide, resulting in decreased neural activation to the diaphragm muscle.
Additionally, when considering the autonomic nervous system, typically individuals who resort to ‘chest breathing’ typically spend more time in a sympathetic “fight or flight” response compared to the vagus nerve driven parasympathetic “rest and digest” response. All this to say, that chest breathing could be correlated to increased stress, risk of anxiety, fainting, and panic attacks, though more research will need to be conducted before conclusions are drawn.
In my practice, I have treated countless patients who experienced positive changes in bowel function (increased frequency and ease of passing bowel movements), ability to empty their bladder, decreased pain with intercourse, resolvement of ‘side stitches’ occurring during running, reduced abdominal bloating, ability to fall asleep, improved core activation, and decreased back pain…just from teaching them how to better utilize their diaphragm muscle! And this is why I’m so passionate about this topic. It’s a simple training that almost every person could benefit from learning!

My Recommendations
Based on the current available research, as well as my own professional experience, here’s what I recommend:
Bras are important for people with breasts, but it must be an appropriately fitting bra. Bras serve to protect the breast tissue and ducts from impact and undue strain. Find out how to fit yourself HERE. And don’t forget: deeply inhale and exhale while trying on a bra or sport bra to ensure it feels comfortable during respiration phase changes.
Recognize that bra size is not consistent across the lifespan as breast size and mass vary throughout life, influenced by hormonal changes (ie. puberty, pregnancy, menopause. This could even be due to a change in hormonal based contraceptives! ), body fat composition, stage of reproductive cycle, and breast pathology.
Do NOT sleep in a bra. Ensure your daughters and granddaughters are not either. Let the thorax and diaphragm have the ability to move without restrictions.
Unless your medical status limits your ability to do so, find a form of activity that makes you breathe at a heavier rate for at least 150 minutes per week, challenging your diaphragm muscle strength and compliance.
Nix wearing tight clothing frequently…yes even those skinny jeans are probably altering how you breathe.
If you would like to be assessed and educated on optimizing the function of your diaphragm by our pelvic health specialist, please reach out via email nomadicphysicaltherapy@gmail.com or text 865-935-9313 for more information
References
Wood K, Cameron M, Fitzgerald K. Breast size, bra fit and thoracic pain in young women: a correlational study. Chiropr Osteopat. 2008 Mar 13;16:1. doi: 10.1186/1746-1340-16-1. PMID: 18339205; PMCID: PMC2275741.
BOWLES, KELLY-ANN1; STEELE, JULIE R.1; CHAUNCHAIYAKUL, RUNGCHAI2. Do Current Sports Brassiere Designs Impede Respiratory Function?. Medicine & Science in Sports & Exercise 37(9):p 1633-1640, September 2005. | DOI: 10.1249/01.mss.0000177590.75686.28 https://journals.lww.com/acsm-msse/fulltext/2005/09000/do_current_sports_brassiere_designs_impede.26.aspx
Dubé BP, Dres M. Diaphragm Dysfunction: Diagnostic Approaches and Management Strategies. J Clin Med. 2016 Dec 5;5(12):113. doi: 10.3390/jcm5120113. PMID: 27929389; PMCID: PMC5184786. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5184786/
Bordoni B, Morabito B. Symptomatology Correlations Between the Diaphragm and Irritable Bowel Syndrome. Cureus. 2018 Jul 23;10(7):e3036. doi: 10.7759/cureus.3036. PMID: 30258735; PMCID: PMC6153095. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6153095/
McGhee DE, Steele JR. How do respiratory state and measurement method affect bra size calculations? Br J Sports Med. 2006 Dec;40(12):970-4. doi: 10.1136/bjsm.2005.025171. Epub 2006 Oct 4. PMID: 17021004; PMCID: PMC2577461. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2577461/
.png)

